Otoplasty (Ear Pinning Surgery)
If you have been self-conscious about ears that protrude, appear oversized, or look uneven, you are not alone. Otoplasty, also known as ear pinning or ear reshaping surgery, is one of the most transformative procedures available for both children and adults who want ears that look proportionate, balanced, and natural. At John Hilinski, MD Plastic Surgery in San Diego, Dr. Hilinski brings a level of specialization in ear surgery that is rare among facial plastic surgeons, offering multiple advanced technique options tailored to each patient’s unique anatomy and goals.
Whether you are searching for otoplasty near you or have been researching ear surgery for years, this page will walk you through everything you need to know, from candidacy and technique to recovery and results.
Dr. Hilinski, Nicole, and team are absolutely amazing! Dr. Hilinski is very knowledgeable, takes the time to thoroughly explain procedures, and has gone above and beyond with patient care during my procedure and throughout all of my follow-ups.
What is Otoplasty?
Otoplasty is a surgical procedure that corrects the size, shape, or position of one or both ears. It is most commonly performed to address ears that protrude significantly from the sides of the head, a condition sometimes called prominauris. However, ear surgery can also address:
- Macrotia (ears that are disproportionately large)
- Asymmetrical ears
- Misshapen or cupped ears
- Earlobes that are stretched, torn, or disproportionately large
- Unsatisfactory results from a previous ear surgery (reverse otoplasty)1
Unlike many practices that offer a single standard ear pinning technique, Dr. Hilinski performs a full spectrum of ear surgeries, including traditional otoplasty, scarless incisionless otoplasty, preservation otoplasty, and macrotia ear reduction. This breadth of technique allows for a truly customized approach that no single-method practice can match.

Who Is a Good Candidate for Ear Surgery?
Otoplasty is one of the few cosmetic procedures commonly performed on children, and for good reason. According to the American Society of Plastic Surgeons, ear cartilage is typically stable enough for surgery by age five or six, making early intervention possible before school-age social pressures begin.2 Adults of any age are also excellent candidates.
You may be a good candidate for otoplasty if you:
- Have ears that protrude excessively from the side of the head
- Are bothered by the size, shape, or symmetry of one or both ears
- Are in good overall health
- Have realistic expectations about surgical outcomes
- Are a child who is at least five years old and can cooperate with post-operative care instructions
A thorough consultation with Dr. Hilinski will determine which technique is best suited to your anatomy and goals.
Otoplasty Techniques Offered by Dr. Hilinski
One of the most significant advantages of choosing Dr. Hilinski for ear surgery in San Diego is his mastery of multiple surgical approaches. Rather than applying a one-size-fits-all method, he selects the technique that will produce the most natural, lasting result for each individual patient.
Traditional Otoplasty (Ear Pinning)
The most widely performed approach, traditional otoplasty involves a small incision placed behind the ear in the natural crease, keeping any scarring completely hidden. Through this incision, Dr. Hilinski reshapes and repositions the ear cartilage, recreating the antihelical fold and reducing the prominence of the conchal bowl as needed. Permanent sutures hold the cartilage in its new position.
Scarless Incisionless Otoplasty
For patients with mild to moderate ear prominence, Dr. Hilinski offers a scarless, incisionless technique performed entirely in the office. This minimally invasive approach uses small, nearly imperceptible access points rather than a traditional incision, resulting in no visible scarring and a significantly faster recovery. It is an ideal option for patients who want meaningful improvement with minimal downtime.
Preservation Otoplasty
Preservation otoplasty is a specialized technique in which the ear cartilage is reshaped and repositioned without being removed. By preserving the cartilage structure, this approach produces a more natural-looking result and reduces the risk of the over-pinned or telephone-ear deformity that can occur with more aggressive cartilage removal techniques.
Macrotia Ear Reduction
Macrotia, or abnormally large ears, is a distinct condition that requires a different surgical strategy than standard ear pinning. Dr. Hilinski is one of, if not, the leading plastic surgeons in the world who specializes in macrotia ear reduction, a procedure that reduces the overall size of the ear while maintaining natural contour and proportion. He has developed a dedicated practice and educational platform around this procedure, reflecting his depth of experience in this area.
Your Consultation
Every otoplasty journey at our San Diego practice begins with a thorough one-on-one consultation with Dr. Hilinski. During this appointment, he will:
- Evaluate the size, shape, position, and symmetry of your ears
- Review your medical history and any prior ear surgeries
- Discuss your aesthetic goals and the outcomes that are realistically achievable
- Explain which technique or combination of techniques is most appropriate for you
- Walk you through the procedure, recovery, and what to expect at each stage
“I always tell patients that the goal of ear surgery is not to make the ears disappear, but to make them stop being the first thing anyone notices,” says Dr. Hilinski. “The best result is one where the ears simply look like they belong.”
The Otoplasty Procedure
Otoplasty is typically performed as an outpatient procedure under local anesthesia. In some cases, patients will elect to have sedation or general anesthesia, depending on the patient’s age and the complexity of the case. The procedure generally takes one to two hours.
For traditional otoplasty, the steps include:
- A small incision is made in the natural crease behind the ear
- The cartilage is sculpted, folded, or reduced to achieve the desired shape and position
- The antihelical fold is recreated using permanent sutures
- The conchal bowl is reduced if it is contributing to ear prominence
- The incision is closed with sutures that are hidden within the crease
Scarring is minimal and concealed behind the ear, making it virtually undetectable once healed.
Recovery and Results
Recovery from otoplasty is generally well-tolerated. Most patients return to light daily activities within one to two weeks following ear surgery, with children typically returning to school within seven to ten days.
What to expect during recovery:
- Days 1 to 3: A soft bandage or headband wraps the ears to protect them and support healing
- Week 1: Mild swelling and bruising are normal; most patients are comfortable with over-the-counter pain relief
- Weeks 2 to 4: A lighter headband is worn at night to protect the ears during sleep; strenuous activity should be avoided
- Month 3: Final results are visible as residual swelling fully resolves
Results from otoplasty are long-lasting. Once the cartilage has healed in its new position, the improvement is considered permanent. Patients consistently report significant improvements in self-confidence and quality of life following the procedure. Patient satisfaction rates following otoplasty are among the highest of any facial plastic surgery procedure.3


Why Choose Dr. John Hilinski for Otoplasty in San Diego
Dr. John M. Hilinski is a double board-certified facial plastic surgeon with a level of dedication to ear surgery that sets him apart from general plastic surgeons in the San Diego area. His credentials and training include:
- Graduate of Harvard Medical School
- Residency in Otolaryngology, Head and Neck Surgery at UC San Diego Medical Center
- Fellowship in Facial Plastic and Reconstructive Surgery
- Double board certification by the American Board of Facial Plastic and Reconstructive Surgery (ABFPRS) and the American Board of Otolaryngology, Head and Neck Surgery (ABOHNS)
- Former facial plastic surgeon for the San Diego Chargers NFL team
- Recognized as a Castle Connolly Top Doctor
- Named a 2024 Top Patient-Rated San Diego Facial Plastic Surgeon by Find Local Doctors
- Over 24 years of experience in facial plastic surgery, with a dedicated focus on ear surgery
Dr. Hilinski’s specialized focus on ear surgery, including his dedicated macrotia surgery platform and his development of advanced incisionless techniques, reflects a depth of experience that is unmatched in the San Diego region.
Patient Reviews and Before and After Results
Patients who have undergone otoplasty with Dr. Hilinski consistently describe life-changing results and exceptional care throughout the process.
“I cannot put into words how thankful I am for Dr. Hilinski and his incredible work. I had ear reduction surgery, and the results completely exceeded every expectation I had. The transformation is unbelievable, so natural, perfectly balanced, and truly life changing.”
– E. Google Review ⭐⭐⭐⭐⭐
“I recently had Ear Reduction surgery done by Dr.Hilinski and I could not be happier. He truly is a master at his craft. He far exceeded my expectations and I have my confidence back. From the moment I had my first consult his staff and clinic were kind and welcoming. Dr. Hilinski has a wonderful bedside manner and was truly attentive and cared to listen. I’m so glad I found him and decided to do this surgery. I couldn’t be happier! Thank you Dr. Hilinski!!!”
– A.S., Google Review ⭐⭐⭐⭐⭐
“Such a positive experience here! We had otoplasty (ear procedure) done for our 5 year old and everything went so smoothly. I did a ton of research beforehand and Dr. Hilinski was highly recommended. I’ve been blown away by the number of pre-op and follow up appointments included as well. The team is so caring and every time we’ve come it’s been fantastic. I knew we were in good hands with Dr. Hilinski and his work is incredible. If you are looking for otoplasty, especially if it’s for your child, I highly recommend him. I’m glad we did it when we did.”
– D.G., Google Review ⭐⭐⭐⭐⭐
“I want to give a huge thank you to Dr. Hilinski and his entire team! I just had macrotia ear reduction surgery a few days ago and I truly couldn’t be happier with the results. He did exactly what I was hoping for. I’ve struggled with feeling insecure about my ears for my entire life. I’m so glad to have found Dr. Hilinski because his expertise and experience on ear reduction surgery are nowhere else to be found! The surgery itself was very comfortable and seamless. Everyone took the best care of me. Dr. Hilinski, your hands are truly blessed!!”
– B.F., Google Review ⭐⭐⭐⭐⭐
Case 15505
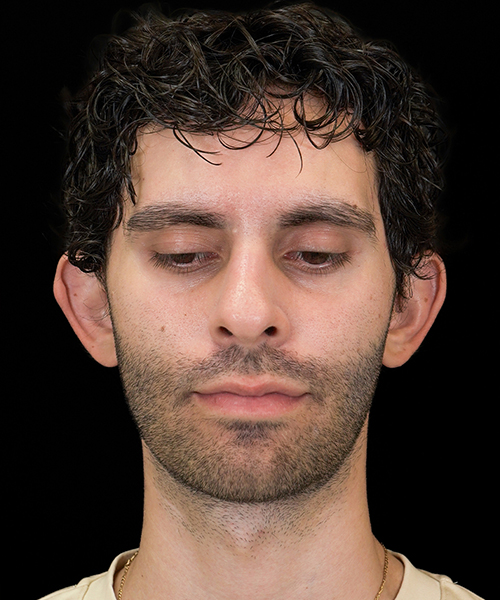

Case 15405


Case 15099

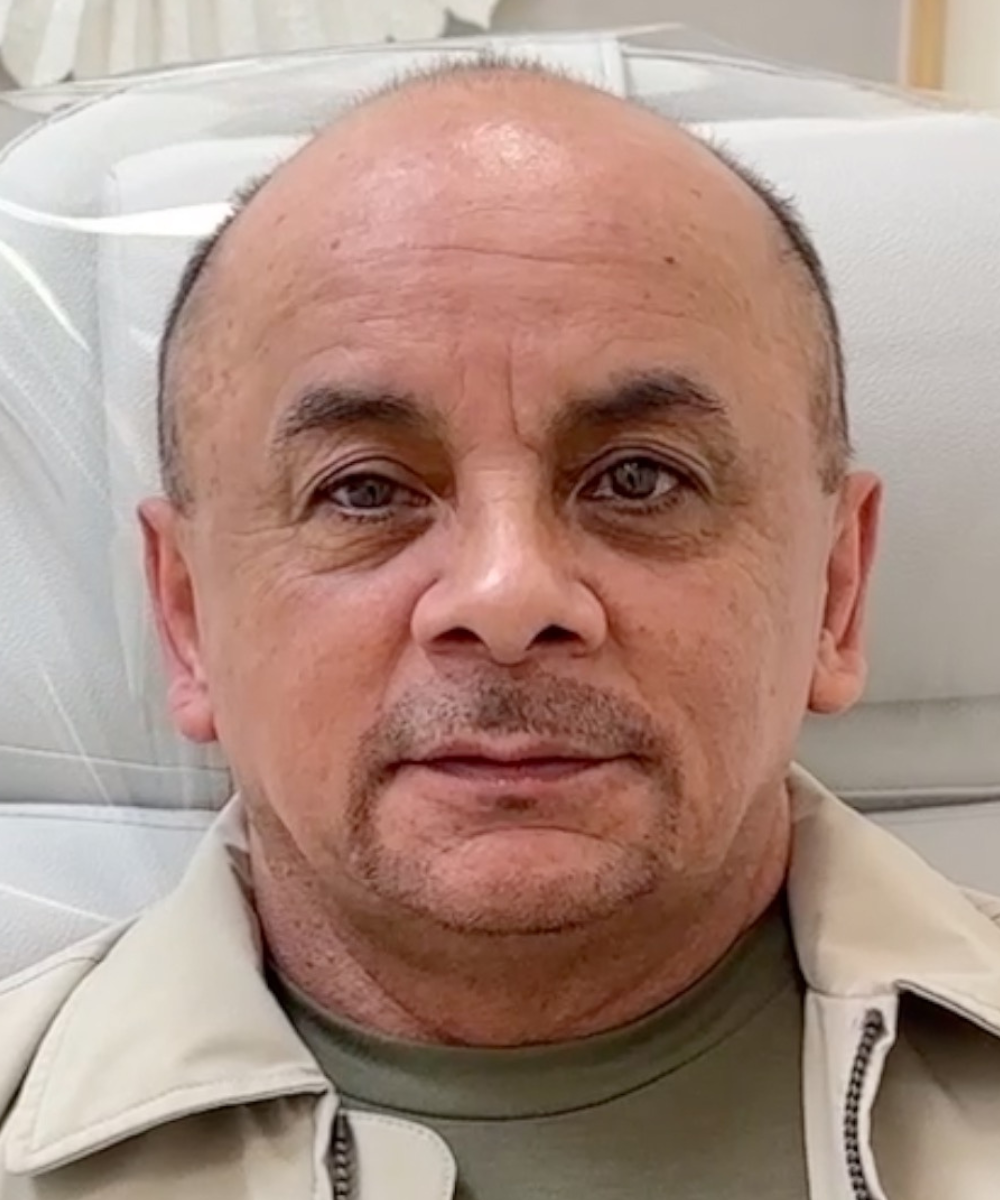
Case 15031
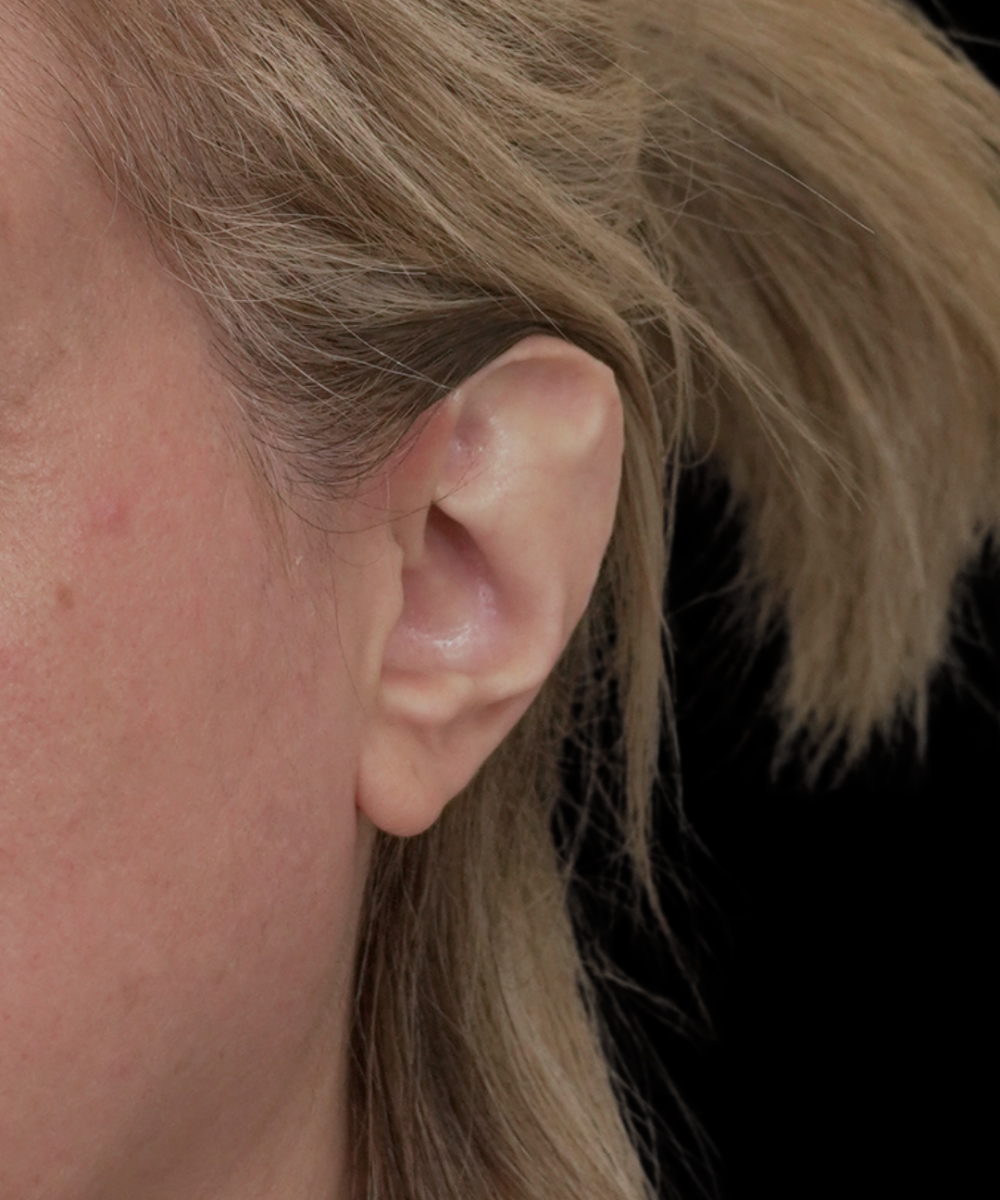
Case 15012


Frequently Asked Questions About Otoplasty
Otoplasty can address a wide range of ear concerns, including protruding or prominent ears, macrotia (oversized ears), asymmetrical ears, misshapen or cupped ears, stretched or torn earlobes, and unsatisfactory results from a prior ear surgery. Dr. Hilinski will evaluate your specific anatomy during your consultation to determine the most appropriate approach.
Yes. Otoplasty is considered safe for children once the ear cartilage has reached sufficient maturity, typically around age five or six. Performing the procedure before a child enters school can help prevent the social and emotional impact of teasing related to ear appearance.
In traditional otoplasty, the incision is placed in the natural crease behind the ear, where any resulting scar is hidden from view. For patients who undergo the scarless incisionless technique, there are no incisions at all, only small needle punctures that heal without visible marks.
Otoplasty results are considered permanent. Once the ear cartilage has healed in its new position, it remains there. Minor changes due to natural aging may occur over time, but the structural correction achieved through surgery is long-lasting.
John Hilinski, MD Plastic Surgery is located in San Diego and serves patients throughout the greater San Diego area. Dr. Hilinski is one of the most experienced ear surgery specialists in Southern California, offering a full range of otoplasty techniques including traditional ear pinning, scarless otoplasty, preservation otoplasty, and macrotia reduction. If you are searching for otoplasty near you, we invite you to schedule a consultation to discuss your goals and learn which approach is right for you.
Yes, the ears will appear overcorrected initially, as they are positioned closer to the head. This is intentional, as the ears will relax into a natural position over the first few months of healing.
Otoplasty results are permanent. The ears will maintain their new shape and position for a lifetime, providing long-term satisfaction.
Contact Us
If you are ready to learn more about otoplasty or ear pinning surgery near you in San Diego, we invite you to schedule a consultation with Dr. John Hilinski. Our team serves patients throughout San Diego, La Jolla, and the surrounding Southern California communities. Take the first step toward ears that feel balanced, proportionate, and naturally yours.
Sources
1 Mayo Clinic. Otoplasty. Available: https://www.mayoclinic.org/tests-procedures/otoplasty/about/pac-20394822. Accessed March 23, 2026.
2 American Society of Plastic Surgeons. Who is a good candidate for ear surgery? Available: https://www.plasticsurgery.org/cosmetic-procedures/ear-surgery/candidates. Accessed March 23, 2026.
3 Eskandari S, Ramirez G, Aderinwale B, Yohannes R, Zabel D. Assessing Patient Satisfaction Following Otoplasty: A Social Media Analysis. Craniomaxillofac Trauma Reconstr. 2026 Feb 6;19(1):11. doi: 10.3390/cmtr19010011. PMID: 41725914; PMCID: PMC12922110. Available: https://pmc.ncbi.nlm.nih.gov/articles/PMC12922110/. Accessed March 23, 2026.
