Functional septorhinoplasty, or functional rhinoplasty, is a term often used to reference several different types of reconstructive nose surgery intended to improve the function of the nose. In essence, it is surgery being performed to help a patient breathe better through their nose. There is a wide variety of techniques that may need to be employed when trying to make the nose function better. This example is presented here because it highlights a number of the most commonly used septorhinoplasty techniques in functional reconstruction of the nose.
Initial Presentation
This particular male patient from San Diego was referred to the office with a chief complaint of difficulty breathing through the nose. Like many patients, he had obstructed breathing on both sides of his nose. This turned out to be the result of a number of anatomical problems with the framework of his nose – meaning, the cartilage structure underlying the nasal skin.
The manifestation of this in terms of appearance can be seen in his preoperative photos shown here. As you can see, his nose is quite asymmetrical, or crooked. In fact, looking at his frontal view, you can see that his nasal bridge deviates off to his right side (left when looking at the photo). On both his oblique and lateral view, the nasal tip appears quite droopy, or ptotic (pronounced ‘tot-ik’).
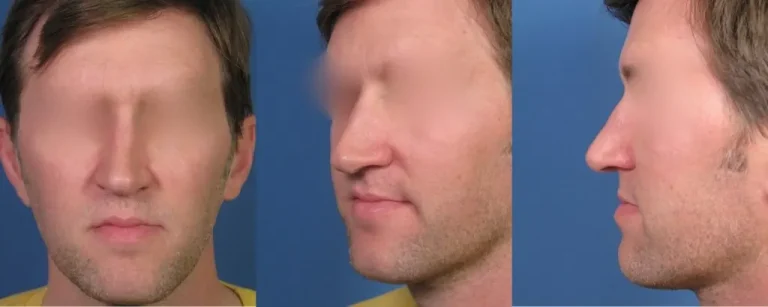
Assessment of Nasal Obstruction
Examining his nose in more detail, there are a number of anatomical problems that needed to be assessed and understood before proceeding with any type of reconstructive surgery. This is where experience in reconstructive nose surgery becomes so critical in terms of achieving a successful outcome.
One thing that is not visible in photos is the presence of a deviated nasal septum. This was initially diagnosed by his primary care doctor before he was referred to my office. My examination confirmed the septal deviation and the need for septoplasty surgery. However, as it turns out, the deviated septum was only one factor when explaining why he had such severe nasal obstruction.
The diagrammed photo provided here helps explain the other issues with the cartilage framework of his nose.
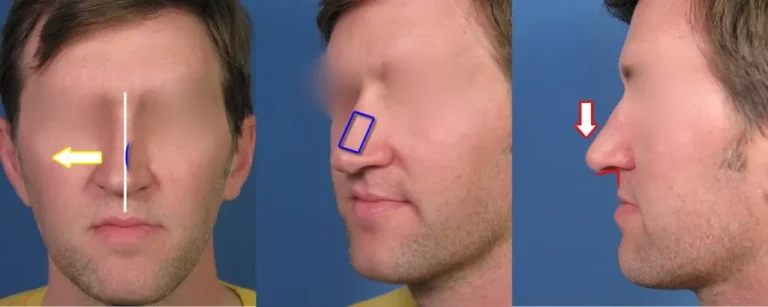
For example, let us go back to his frontal view. The white vertical line in the diagram indicates where the bridge of the nose really should be aligned in terms of the middle of his face. Instead, you can appreciate how a majority of his nose appears displaced to his right side as noted previously. This visual illusion is primarily due to the fact his nose is collapsed through the middle one-third as indicated by the curved blue line. This actually corresponds to a critical area of the nose often times referred to as the ‘middle vault’ or ‘internal nasal valve area’ by rhinoplasty experts. The middle vault and internal nasal valve are discussed in more detail in our rhinoplasty tutorial chapter on spreader grafting. But suffice it to say that a collapsed middle vault or internal nasal valve, as in this case, can be a significant factor when it comes to difficulty breathing through the nose. In addition, a collapsed middle vault can contribute to visual asymmetry when it comes to the appearance of the bridge as is shown here.
On the oblique view of his nose, you can see how the collapsed middle vault gives the illusion that this side of the nose is relatively flat (as shown by the blue rectangular outline). This is because the upper lateral cartilage, which is a key component of the middle vault anatomy, is depressed toward the opposite side of his nose. Thus, when looking at the nose from this angle, indeed, it does appear somewhat flat.
When looking at his nose from the profile view, you can also sense how the tip of the nose is mild to moderately ptotic, or droopy. This can be confirmed by looking more closely at the nasolabial angle (the angle created by the junction of the upper lip and the bottom of the nose). Normally the nasolabial angle should be around 90-95 degrees in a male. In this particular case, the nasolabial angle is less than 90 degrees. So what does this mean in terms of nasal function and breathing? In many cases, a ptotic nasal tip can contribute to some degree of nasal obstruction. In severe cases of nasal tip ptosis, this can be one of the major factors in terms of obstruction. But it does not have to be severe to negatively impact one’s breathing. Even in cases such as this one, mild to moderate nasal tip ptosis can be a relevant factor that needs to be addressed in order to help improve nasal function. By simply lifting the nasal tip up several degrees (increasing the rotation of the nasal tip), some patients will note moderate to significant improvement in their nasal breathing. Go ahead and try this with your nose – you will note that by lifting the tip slightly (especially if you have nasal tip ptosis) you can breathe easier. It just so happens that lifting the nasal tip up can also improve the aesthetic appearance of the nose in many cases.
Nasal Shape and Functional Improvement
This is a great example of a patient where the nasal shape is going to passively change in concert with functional improvement of the nose. There are a good number of patients who require functional improvement of then nose, but the shape of their nose will change very little. This is because some types of anatomical obstruction of the nose can be corrected without having to reshape the nose. For instance, traditional septoplasty surgery does not have any significant impact on the external appearance of the nose. But in this particular case, because he has significant collapse of the middle vault and ptosis of the nasal tip (with both contributing to obstruction), the corrective nose surgery cannot be done without changing the shape of the nose. In fact, this is an issue that should be openly discussed with patients undergoing this type of reconstructive surgery since they should be fully aware there are passive changes that will occur in the process of improving the nasal function.
Insurance Coverage for Septorhinoplasty
Because one of the main goals of septorhinoplasty is to improve nasal breathing, some patients explore insurance reimbursement for the functional portion of surgery. In select cases, patients with PPO insurance plans may be able to recuperate part of their out-of-pocket costs by submitting a claim directly to their carrier. While our office does not bill insurance for these procedures, we can provide the appropriate documentation if you choose to pursue reimbursement independently. Coverage varies by plan and medical necessity criteria, so patients are encouraged to confirm eligibility and requirements with their insurance provider.
Functional Septorhinoplasty
In this particular case, an open septorhinoplasty procedure was performed. This means that an incision was made between the nostrils extending into the nose on both sides. This allowed for the skin of the nose to be lifted up, thus exposing the cartilage framework of his nose.
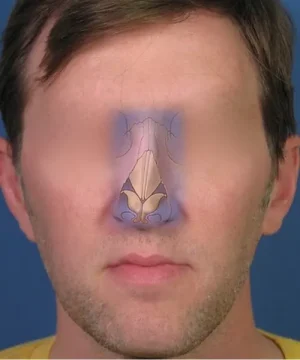
Upon opening the nose, it was readily appreciated that his middle vault was displaced to his right side. This is represented here in the adjacent photo diagram where you can see that his nasal bones were actually quite symmetrical. The issue with his crooked bridge alignment was not a result of displacement of the nasal bones, which is a very common issue that I encounter in my rhinoplasty practice. The crooked alignment was, instead, largely a direct result of the cartilage being pushed off to his right side. Because the middle portion of the bridge was displaced, the nasal tip cartilage followed suit also going off to his right side. What this told me during the surgery was that I did not have to break his nasal bones in order to improve the alignment of his bridge. In order to help correct the anatomical problem, I had to focus on the middle vault of the nose, which was comprised of the paired upper lateral cartilages and the dorsal septum.
Ultimately, as was planned, I ended up placing a layered spreader graft on his left side to correct the problem. Spreader grafting is a very valuable technique that I happen to use quite frequently in my rhinoplasty and revision rhinoplasty practice. You can read more in detail about spreader grafting using this link here to our rhinoplasty tutorial chapter focusing on reconstruction of the middle nasal vault. For the sake of brevity, spreader grafting is an advanced rhinoplasty technique that involves placing a segment of cartilage in a strategically located position, which helps to open up the internal nasal valve. In the process of doing so, spreader grafts can also help to augment (build up) one side (or both if desired) of the nasal bridge to add width. If a spreader graft is created so that it extends further toward the nasal tip (called an extended spreader graft), it can be used to straighten the nasal bridge and tip. That is precisely what was done in this case example.
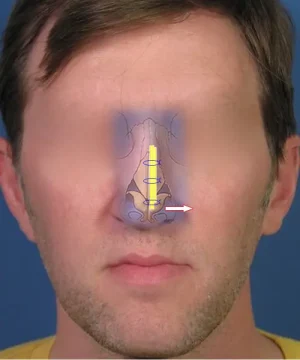
In the adjacent photo diagram the spreader grafts are represented by the yellow shaded rectangles. In fact, in this case, I ended up using three spreader grafts made from harvested septal cartilage sewn together as one, thick layered graft. In doing so, I was able to create a very stiff, moderately thick splinting graft that was resilient enough to help straighten a fairly crooked bridge. The blue ovals represent the sutures used to fixate the graft in position. If you look closely, the upper end of the spreader graft actually extends just underneath the inferior edge of the nasal bone. It then extends along the left side of the nasal bridge into the tip region. As the sutures were sequentially placed from top to bottom, I was able to draw or pull the cartilage framework of his nose toward his left side (as indicated by the arrow). The end result as you can see in the diagram, is restoration of a straighter cartilage alignment – thus providing him an improved and more symmetrical bridge. In terms of the internal valve itself, this type of triple layered spreader graft helped to open up the cross sectional area of the internal valve inside of his nose, contributing to a marked improvement in nasal function.
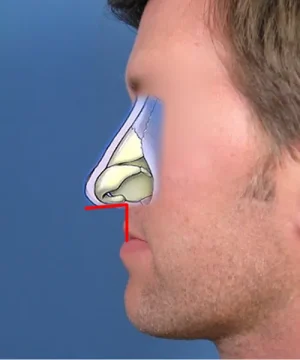
In terms of his nasal tip region, I mentioned earlier how his tip was quite ptotic and contributed to some of his nasal obstruction. Looking at the underlying cartilage framework of his tip (as diagrammed here), you can see how the lower lateral cartilage is the primary problem. The lower lateral cartilage refers to the pair of wings that essentially make up much of the nasal tip shape and support. When the lower lateral cartilages are not positioned correctly, as is the case here, they can give the appearance the nasal tip is drooping down. Functionally, this can be a key factor in patients who cannot breathe optimally through their nose. Once I opened this patient’s nose in surgery, it was confirmed that the lower lateral cartilages needed to be reshaped in order to improve his breathing. In situations like this, the entire nasal tip is deconstructed by separating the lower lateral cartilages – basically detaching them from the rest of the nose. They are then moved to a more ideal position and anchored in their new location using long-term sutures.
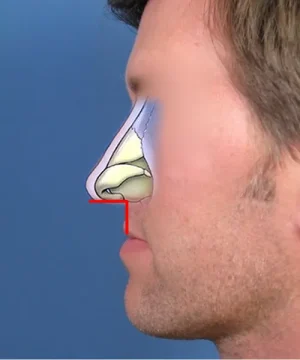
This technique is commonly referred to as a tongue-in-groove maneuver where the medial crura on both sides (forming a groove) are repositioned on the caudal septum (the tongue). In fact, this is a powerful rhinoplasty technique that is used quite frequently in my practice. The overall effect is shown visually in the adjacent diagram where you can now see the nasolabial angle has been opened up to nearly 90 degrees. Comparing the two side views of the cartilage framework, you can appreciate in the after photo the difference in shape and position of the lower lateral cartilage. You can also get the sense that the lower lateral cartilage volume (width) has been decreased in this process. By lifting the nasal tip up using this type of surgical technique, this patient was provided the opportunity to breathe much better. Passively, the nasal tip also appears more esthetically pleasing because there is now less of a droop.
Results of Functional Septorhinoplasty
In the end, this patient benefitted greatly from the reconstructive septorhinoplasty in terms of nasal function. He was able to breathe better out of both sides of his nose largely due to the septoplasty (septal reconstruction), spreader graft placement and correction of the nasal tip ptosis.
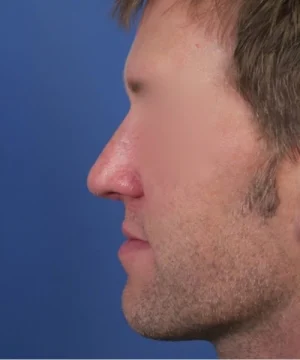
In addition, he had passive changes to the appearance of his nose that are shown here. Overall, you can see that his nose is now much straighter on his face with marked improvement in terms of symmetry. And keep in mind that the nasal bones were not broken during his surgery. The improvements noted in his alignment are a direct result of the middle vault reconstruction using the layered spreader grafting techniques explained above.
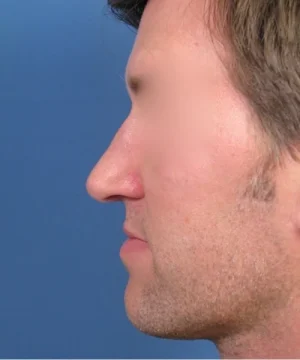
On his oblique (45 degree angle) views, you can also see how much change there has been in the nasal tip region. His nose is now shorter in terms of overall length because the nasal tip has been lifted up to a more ideal position. By doing this in combination with placement of the spreader grafts, his left oblique view shown here has been improved significantly. These same changes carry through to his profile view as well where you can now see his tip is more optimally shaped and positioned. He still maintains a very nice, masculine profile. But this new nose of his now looks and functions much better.




Functional Septorhinoplasty Consult
If you have significant trouble breathing through your nose and feel as if functional septorhinoplasty may benefit you, do not hesitate in contacting my San Diego office today. I am considered one of the regions foremost experts in functional, reconstructive nose surgery.
